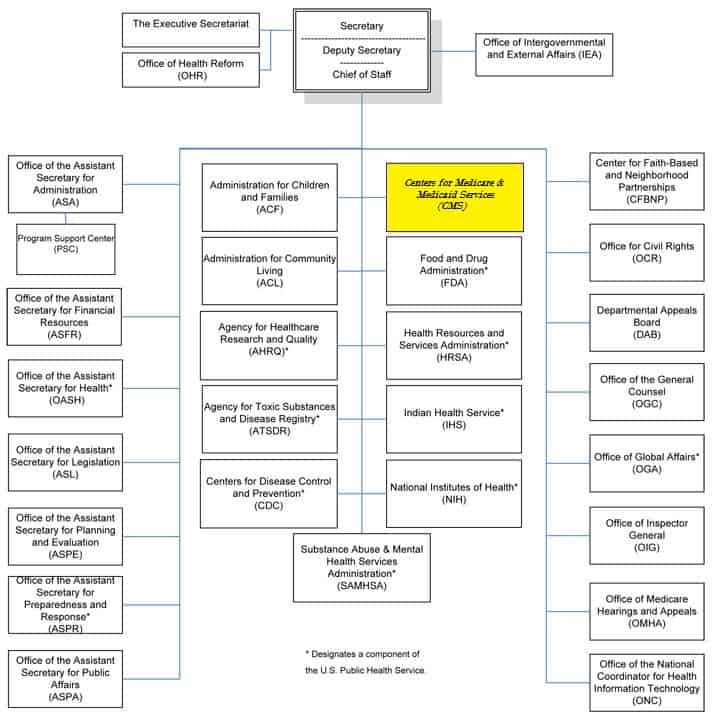
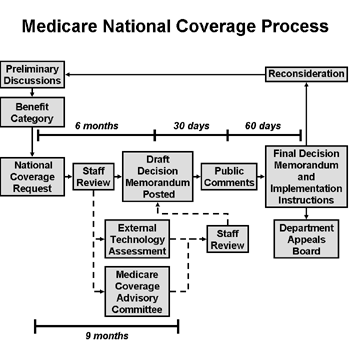
40 medicare appeal process diagram
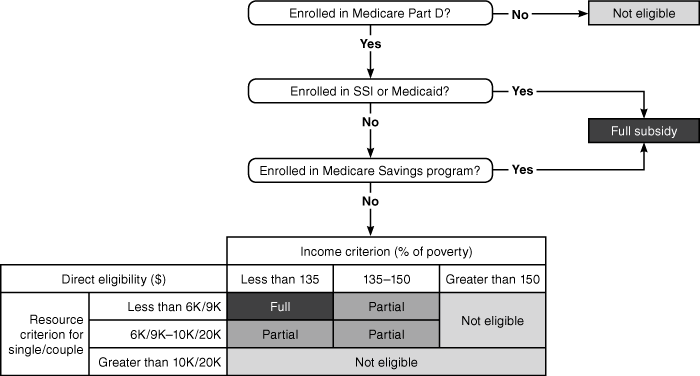
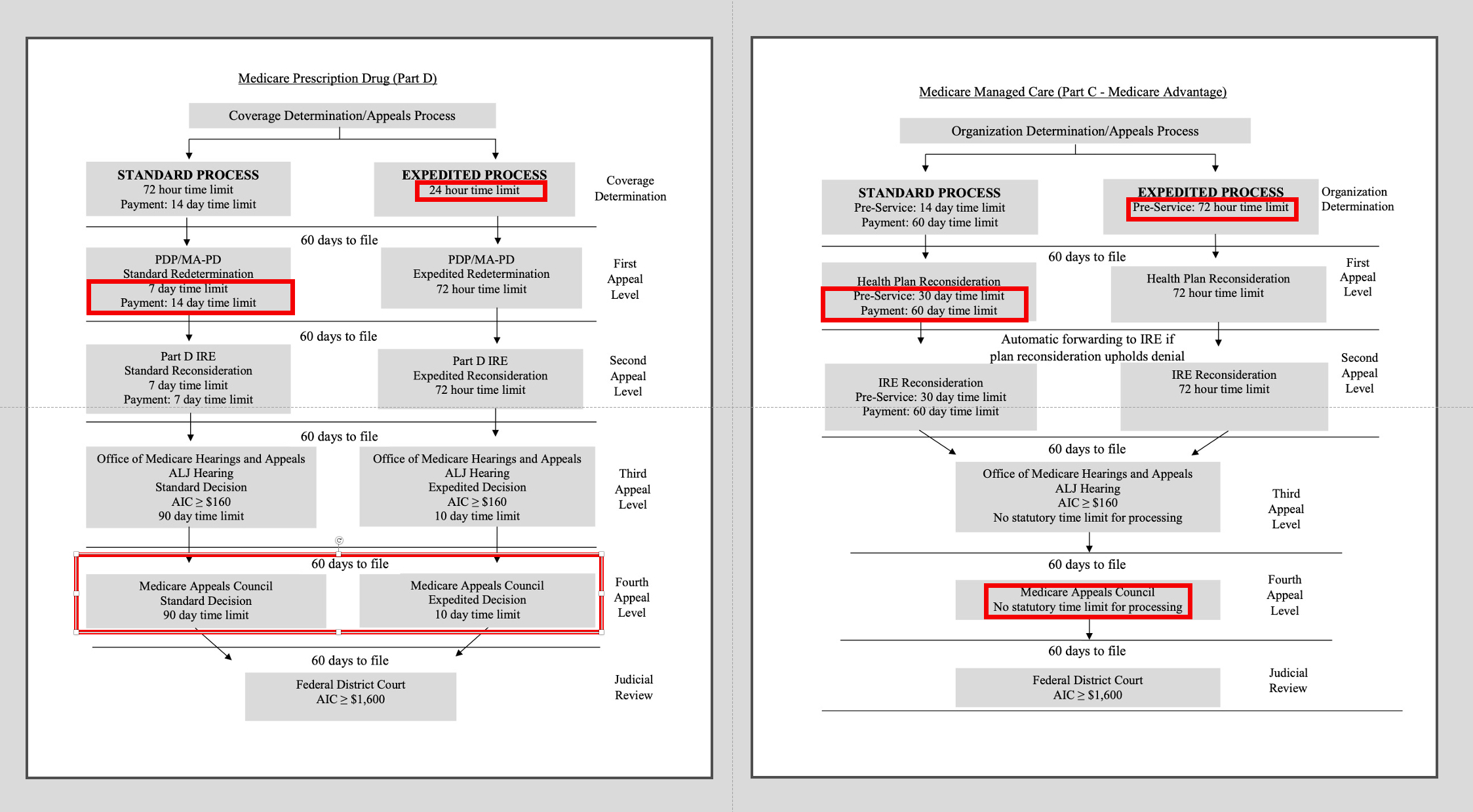
Misalignments in Medicare and Medicaid Appeals Processes The considerable differences between Medicare and Medicaid appeals processes create two distinct paths that Medicare-Medicaid enrollees must navigate when care is denied (Exhibit 1). While new, fully integrated models of care can be designed to offer an aligned appeals process, in most states
an appeal no matter how you get your Medicare. For more information, visit Medicare.gov/appeals, or call 1-800-MEDICARE (1-800-633-4227). TTY users can call 1-877-486-2048. Can someone file an appeal for me? If you want help filing an appeal, you can appoint a representative. Your representative can help you with the appeals steps explained
A third level appeal is a bit more interesting as it requires the hearing to be held over the phone, and at times may require a video teleconference; although extremely rare, it may even be in person. Fourth level of appeal . Fourth level appeals are reviewed by the Medicare Appeals Council within the Department of Health & Human Services.

Medicare appeal process diagram
— Medicare Appeals Council. If you disagree with the ruling from the previous step, then you can file an appeal to the Medicare Appeals Council. Again, this is the next step regardless of which type of Medicare plan that you have. This council is part of the Department of Health and Human Services (HHS) Appeals Board.
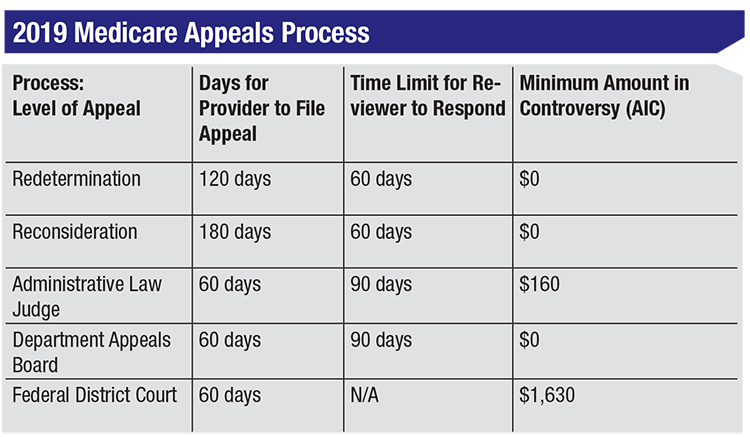
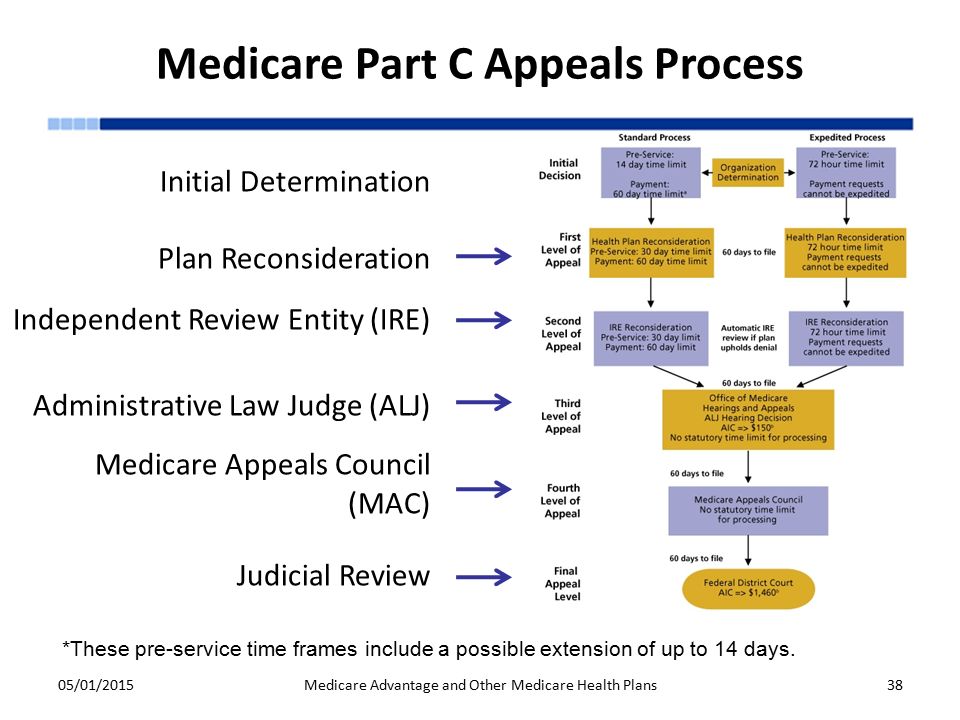
Medicare Hearin gs and A ppeals ALJ Hearing AIC ≥ $180** No statutory time limit for processing . Medicare Appeals Council . No statutory time limit for processing . F. ederal District Court AIC ≥ $ Review1,760** First Appeal . Level Second Appeal Level Third Appeal Level Fourth Appeal Level Judicial
Medicare Parts A & B Appeals Process MLN Booklet Page 6 of 17 MLN006562 May 2021. Appointing a Representative. A party may appoint an individual, including an attorney, at any time to represent them during the claim or appeal process. To appoint a representative, the party and representative must complete the .
Medicare appeal process diagram.
The 5 Levels of the Appeals Process. There are 5 levels of appeals available to you: Redetermination. Reconsideration. Administrative Law Judge (ALJ) Departmental Appeals Board (DAB) Review. Federal Court (Judicial) Review. Level 1 is a Redetermination, which is conducted by the DME MAC. A Redetermination is a completely new, critical re ...
A Guide to Medicare Advantage Appeals. So you've had a claim denied by your Medicare Advantage Plan. Before you throw in the towel and pay for the denied service yourself, you should consider filing an appeal. Medicare Advantage appeals are a process that Medicare beneficiaries can use to appeal Medicare decisions about their Medicare coverage.
You agree to take all necessary steps to insure that your employees and agents ... determination that reach Level 3 of the Medicare claims appeal process.
If you have a Medicare health plan, start the appeal process through your plan. Follow the directions in the plan's initial denial notice and plan materials. You, your representative, or your doctor must ask for an appeal from your plan within 60 days from the date of the coverage determination.
Settled appeals are dismissed Step 10 CMS sends fully executed agreement and Settlement Step 11 Yes Process Over CMS, Appellant & MAC develop consensus Spreadsheet Step 5 Is consensus reached? No Yes Process Complete Low Volume Appeal Settlements Appellant Process Diagram Within 30 days Within 15 days Within 180 days Within 30 days Within 15 ...
AIC = Amount In Controversy. ALJ = Administrative Law Judge. MAC = Medicare Administrative Contractor. *The AIC requirement for an ALJ hearing and Federal ...
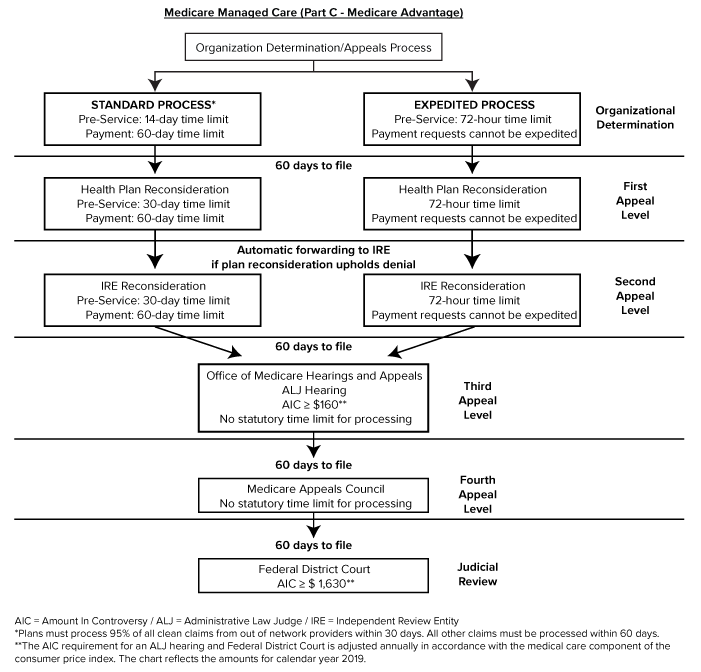
Your Level 1 appeal ("reconsideration") will automatically be forwarded to Level 2 of the appeals process in the following instances: Your plan does not meet the response deadline. If your Medicare Advantage plan fails to meet the established deadlines, it is required to forward your appeal to an independent outside entity for a Level 2 review.
Gov Flowchart – https://www.cms.gov/Medicare/Appeals-and-Grievances/ ... Inpatient hospital services (note: the appeals process for Inpatient Hospital ...
Here's how Medicare beneficiaries can appeal income-related charges that result in higher premiums Published Wed, Nov 10 2021 12:25 PM EST Updated Wed, Nov 10 2021 12:30 PM EST Sarah O'Brien ...
Aug 25, 2020 — Flowchart for Medicare Part D Appeals and Grievances ... Issued by: Centers for Medicare & Medicaid Services (CMS). Issue Date: January 01, ...
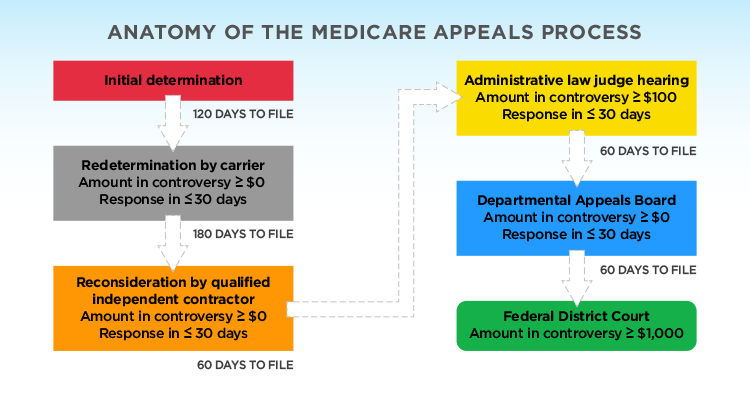
The Five Levels of Medicare Appeals . There are five levels in the Medicare appeals process. If at any time your appeal is approved by Medicare, the process ends at the level you are currently on. If a denial is upheld, you will have to decide whether or not to proceed to the next level.
The Medicare Appeals Process. The Medicare Appeals Process. fAct Sheet. Overview. Section 1869 of the Social Security Act and 42 C.F.R. Part 405 Subpart I contain the procedures for conducting appeals of claims in Original Medicare (Medicare Part A and Part B). There are five levels in the claims appeals process under Original Medicare: 1.
The Medicare Appeals Process fact sheet (ICN 006562) is available in a downloadable format. This fact sheet is designed to provide education on the five levels of claim appeals in original Medicare (Medicare Part A and Part B). It includes details explaining how the Medicare appeals process applies to providers, participating physicians, and ...
The appeals process has five levels. The first level asks Medicare or your Medicare health or prescription drug plan for a "redetermination" on the original request. If your first-level appeal is denied, you may appeal to the next level and the next.
Medicare health plans, which include Medicare Advantage (MA) plans - such as Health Maintenance Organizations, Preferred Provider Organizations, Medical Savings Account plans and Private Fee-For-Service plans - Cost Plans and Health Care Prepayment Plans, must meet the requirements for grievance and appeals processing under Subpart M of the Medicare Advantage regulations.
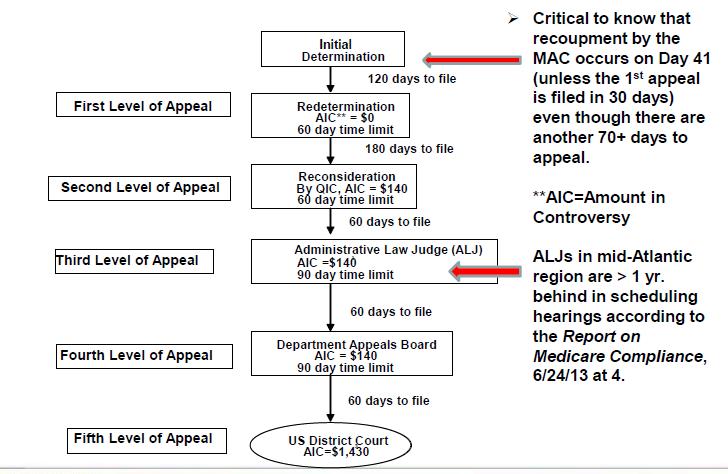
medicare appeals process The third level and beyond Under both the previous and new appeals systems, the third level of appeal is an administrative law judge (ALJ) hearing, and physicians have 60 ...
MEDICARE PART A APPEALS PROCESS. Definition of Appeals. An appeal process is available to providers who are dissatisfied with the determination rendered on their claim. The process consists of five levels. Each level is discussed in detail below. Each level must be completed for each claim at issue prior to proceeding to the next level of appeal.
If you disagree with your plan's initial decision, you can file an appeal. The appeals process has 5 levels. If you disagree with the decision made at any level of the process, you can generally go to the next level. At each level, you'll get instructions in the decision letter on how to move to the next level of appeal.
Keep copies: Be sure to keep a copy of everything you send to your plan as part of your appeal. Start the process: Follow the directions in your plan's initial denial notice and plan materials. You have 60 days from the date of the coverage determination. If you miss the deadline, you must provide a reason for filing late.
The Medicare appeals process has five levels. If you disagree with a decision made at any level of the appeals process, you can generally go to the next level to make your claim. As you go through the process, you'll receive instructions in the decision letter on how to move on to the next step of the process.
Standard Medicare Appeal Letter Templates. Item #: N/A Type: PDF. Download our Standard Medicare appeal letter templates to help you more quickly submit an appeal and ensure you include all necessary information the first time. There is an appeal letter template for each of the five levels of a Standard Medicare appeal process.
Jul 27, 2018 — Once an initial claim determination is made, beneficiaries, providers, and suppliers have the right to appeal Medicare coverage and payment ...
To see a diagram (flowchart) of the original Medicare (fee-for-service) standard and expedited appeals process, go to the "Downloads" section below. Appointment of Representative A party may appoint any individual, including an attorney, to act as his or her representative during the processing of a claim(s) and /or any claim appeals.
The Medicare Advantage appeals process includes four levels of review by several entities. At each level of review, a denied claim may be overturned, partially overturned, or upheld. The Center for Medicare and Medicaid Services (CMS) refers to the insurance company and the Medicare Advantage plans they promote as Medicare Advantage ...
• A ll appeal requests must be made in writing. Five Levels in the Appeals Process Medicare offers five levels in the Part A and Part B appeals process. The levels, listed in order, are: • Redetermination by an FI, carrier or MAC • Reconsideration by a QIC • Hearing by an Administrative Law Judge (ALJ) •
Departmental Appeals Board (DAB) Review/Appeals Council. 60 days from the date of receipt of the ALJ decision/dismissal. None. Federal Court (Judicial) Review. 60 days from the date of receipt of the Appeals Council decision or declination of review by DAB. For requests filed on or after January 1, 2021, at least $1,760 remains in controversy*.
Check your claim status with your secure Medicare account, your Medicare Summary Notice (MSN), your Explanation of Benefits (EOB), Medicare's Blue Button, or contact your plan. File an appeal. How to appeal a coverage or payment decision made by Medicare, your health plan, drug plan or Medicare Medical Savings Account (MSA) Plan.
There are five levels of a Medicare appeal: (1) redetermination, (2) reconsideration, (3) hearing, (4) review, and finally (5) judicial review in federal district court. Each level of the appeal process has its own requirements and time limits for filing.




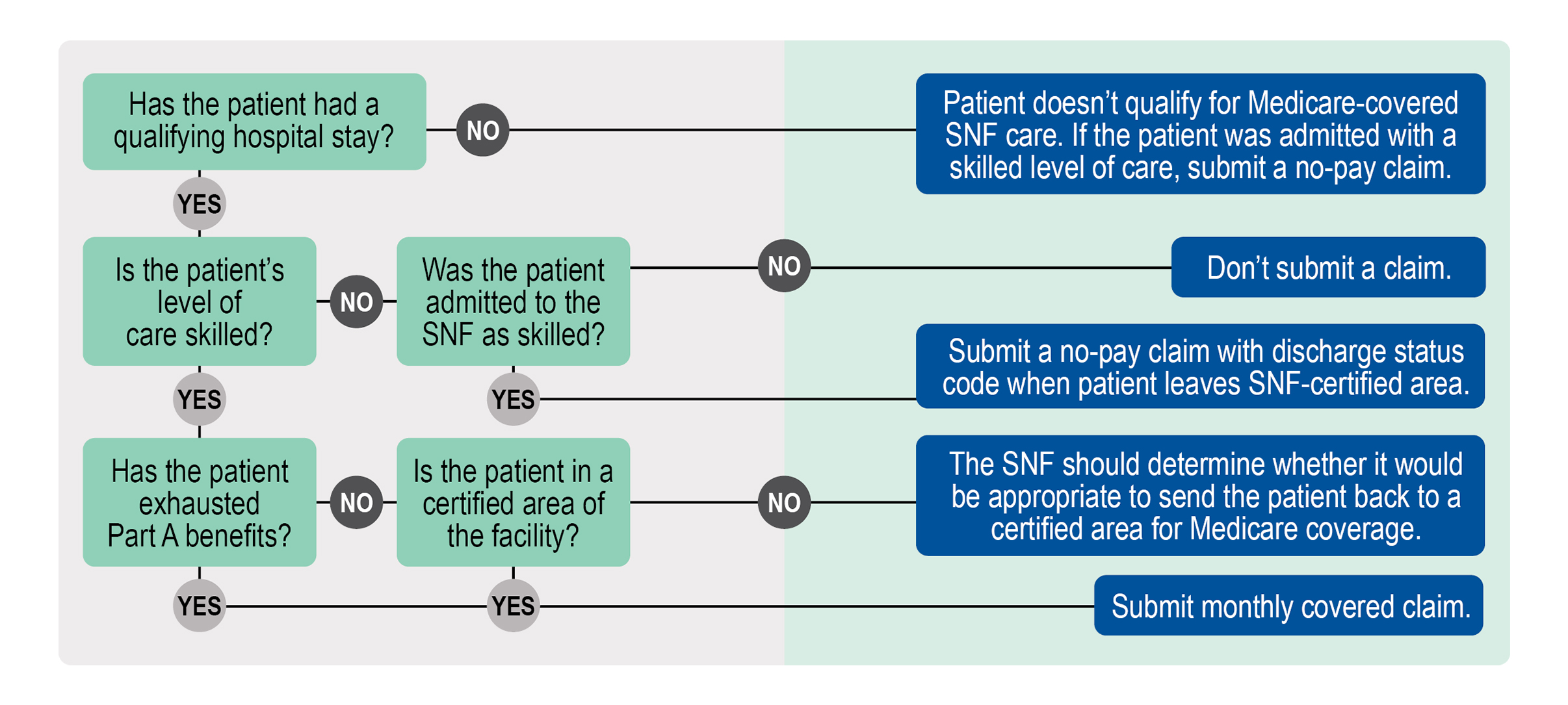
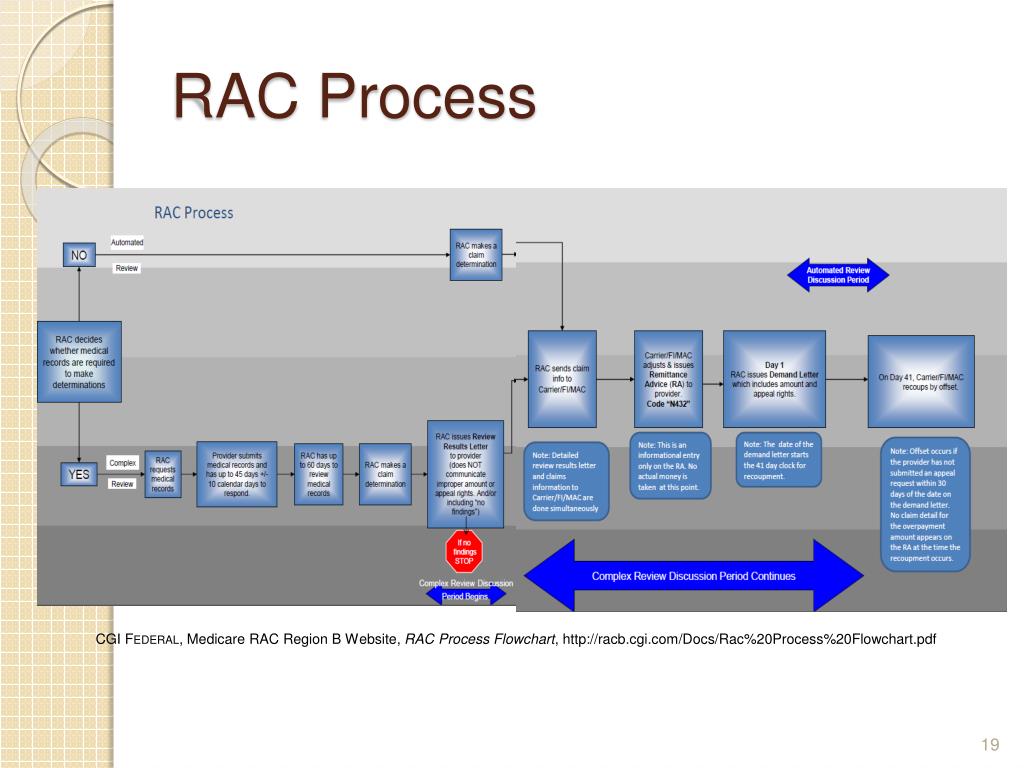
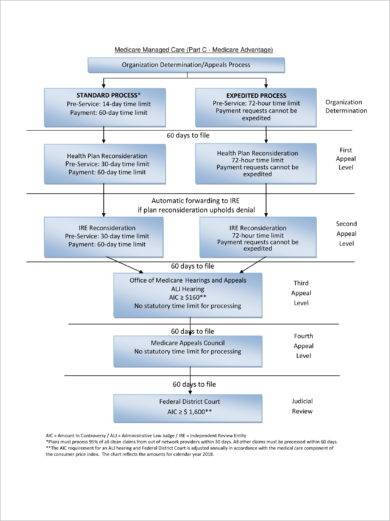
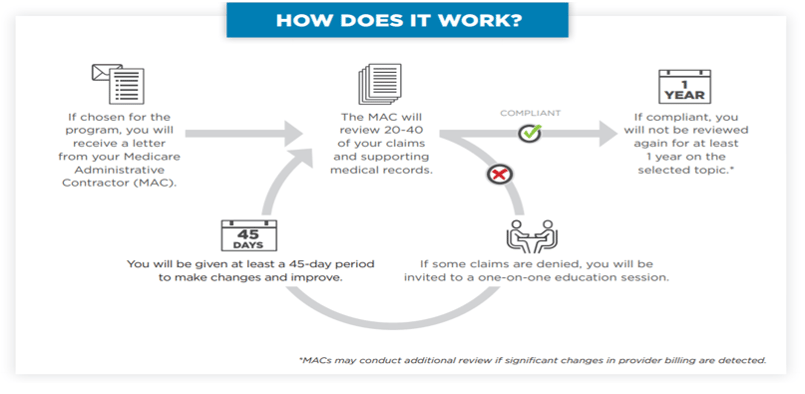










0 Response to "40 medicare appeal process diagram"
Post a Comment